Hello everyone!
The Group Luncheon will be on May 10, 2019 (5/10/2019) at 1pm. Please meet at Danny’s Restaurant.
Address:
3715 Genesee Street
Cheektowaga, NY 14225
You can access their lunch menu here
Hello everyone!
The Group Luncheon will be on May 10, 2019 (5/10/2019) at 1pm. Please meet at Danny’s Restaurant.
Address:
3715 Genesee Street
Cheektowaga, NY 14225
You can access their lunch menu here
There is a Facebook group devoted to aphasia call the Aphasia Recovery Connection. It’s open to SLP’s, caregivers & people with aphasia. It’s a closed group so you have to go through a brief but simple process to join the group. Join me there since I think I might be the only one of more than 8000 members worldwide who’s from Buffalo.
Also UB Neurosurgery has a brain aneurysm support group at this link.
“Helen Wulf, stroke survivor and person with Aphasia, provides an extremely rare and personal glimpse into what it,s like to live with Aphasia, or the loss of access to the language network of the brain after a brain injury. She wrote this book after dedicating year to her stroke recovery.”
The following are the 10 quotes from her book. “The speech therapist help the patient feel excitement in making the slightest progress. It is easy for the patient to set unattainable goal for himself and the therapist is invaluable in helping him realize that progress is made in turtle steps. Smiles and touches do wonders. Happy laughing heals.”
“Verbal communication, speaking, and interpreting, is so vital to being human that many assume when one loses that ability one lose his mind. His mind is still churning, probably working overtime. It’s his brain that’s been bashed.
I feel wonderful about coming to therapy because at first I couldn’t do these things that I can do now. Before coming to therapy, I couldn’t do things like speaking words as much as I do now. I think that’s because of Kristen, the student clinician and the hard work that I have put in.
Saleemah
Hi Everyone!
As a reminder, during our group on Friday, May 3rd, we will be having a certified therapy dog, Stella, and its owner, Dr. Krista Garland, come in and give us a presentation about the benefits of therapy dogs. Again, this group is completely optional, as we want everyone to feel safe and comfortable.
Dr. Garland is an associate professor at Buffalo State in the Exceptional Education Department. Her dog, Stella, holds “office hours” on campus every Friday, so students can come visit her. Dr. Garland describes her dog as “a natural” and states Stella works well with new people.
Dr. Garland and Stella volunteer through Paws for Love, a program through the SPCA. Through this program, owners bring their cats or dogs to areas around the Buffalo area, such as nursing homes, group homes, assisted living facilities, and colleges.
For further information regarding Paws for Love, visit their website.
-Olivia
Did you know there is an online community of brain injury survivors from around the world? There is, and it’s all centered around a podcast. The NeuroNerds podcast addresses two of my favorite things: surviving a stroke & the Marvel Cinematic Universe. The hosts are stroke survivor Joe Borges and concussion survivor Lauren Manzano. Every week, the podcast features a new brain injury survivor, and a new brain injury charity and chat about nerdy subjects. For more information on the NeuroNerds click on this link.



Everyone’s aphasia is different and manifests in different ways. If everyone’s aphasia was the same, it might be simpler for SLP’s to treat it! But alas, everyone’s aphasia is different. My own aphasia goes something like this:
I can read and write just fine. Some people with aphasia have trouble reading or writing (or some combination or the two), some do not.
I can speak in complete sentences. (People with aphasia have varying degrees of difficulty with speech. We haven’t lost our intellect.)
I have trouble explaining complex concepts extemporenously.
I have difficulty concentrating and my mind often goes blank.
I have great difficulty multitasking, and easily get overwhelmed.
I have problems working and trying to speak while under pressure.
That’s my aphasia. What is your aphasia like? Write it in the comments or in a blog post.
Lauren Marks’ Recovery Story from Brain Anuersym/Aphasia
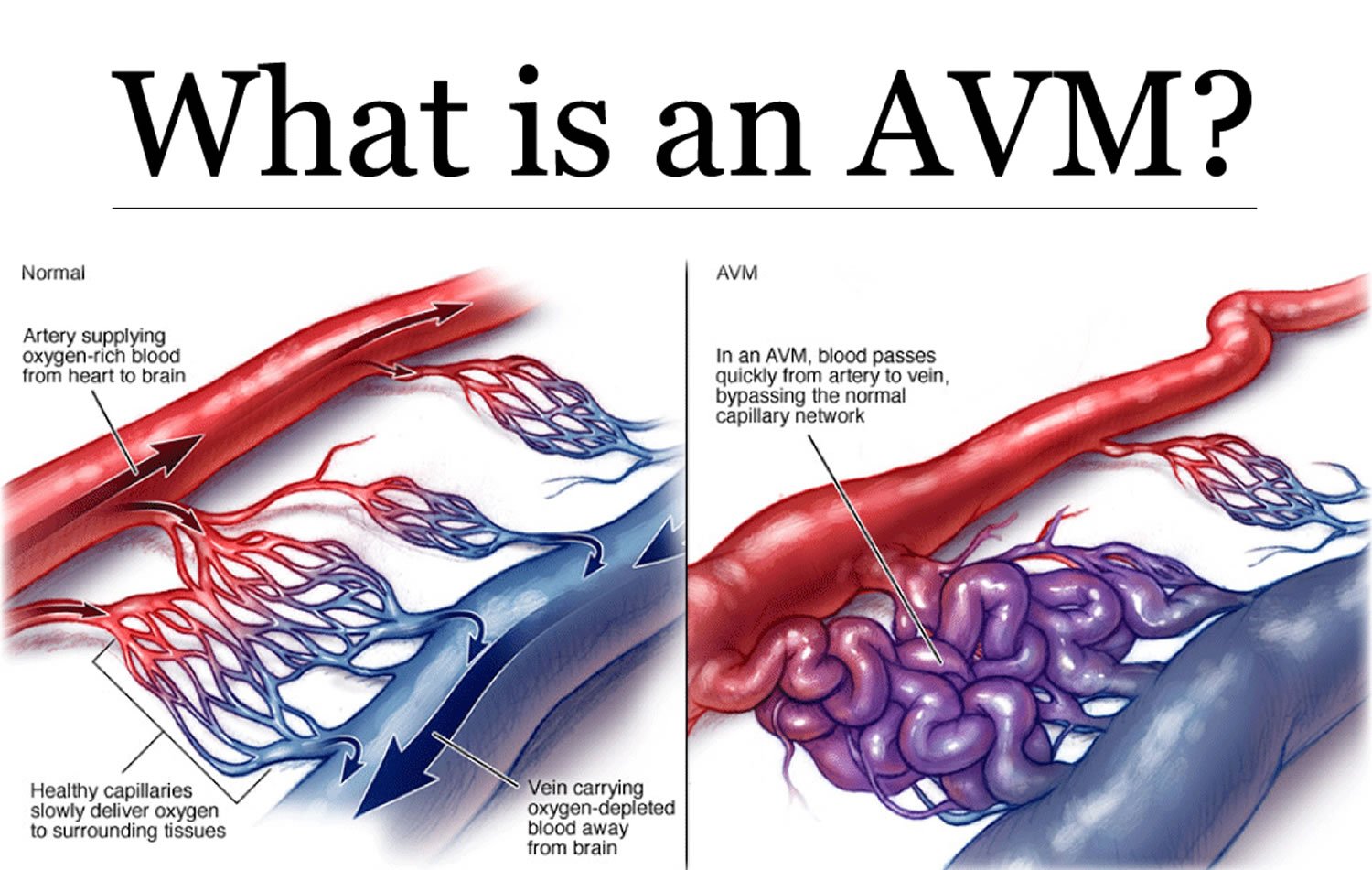
I had an Arteriovenous Malformation (AVM), a type of fistula of the brain that had to be resected via craniotomy. The only good thing is that, unlike most people that have this type of open brain surgery, I had the craniotomy done the very next day after diagnosis – which left me little time to get scared or freaked out.
On the morning of December 10, 1996, Jill Bolte Taylor, a thirty-seven year old Harvard trained brain scientist, experienced a massive stroke when a blood vessel exploded in the left side of her brain. A neuroantomist by profession,she observed her own mind completely deteriorate to the point that she could not walk, talk, read, write, or recall any of her life, all within the space of four brief hours.
In My Stroke of Insight, Taylor shares her unique perspective on the brain and its capacity for recovery, and the sense of omniscient understanding she gained from this unusual and inspiring voyage out of the abyss of a wounded brain.
Saleemah
My stroke story begins on a nice fall day, Wednesday October 3, 2018. My normal routine on a Wednesday was to get up early and go to the Hamburg Chamber breakfast meeting at 730am at a cafe in Hamburg. After an enjoyable social, I left at 930am and began to drive towards home. As I was driving, I noticed my mind and my thoughts begin to slow. I was slowly losing strength in my right hand, arm, and leg. I made a decision to drive over to the VA hospital. My driving began to slow down and get slower as I went along. I realized I was getting worse. A lady pulled up to the left of my vehicle and called to me to pull over because I was driving too slow. I pulled my car off Harlem Rd. to a side street and parked. The lady called 911 and an ambulance came and took me to the GVI at Buffalo General Hospital. I was diagnosed with a left hemorrhagic stroke and was taken to surgery to have the blood removed. The surgeon was pleasantly surprised to see that I was able to speak at all and understand most of what he said to me! After one week, I was moved to the rehab unit in the hospital for two weeks. I began speech therapy at the VA hospital twice a week in November to learn my words again.
Hello everyone, it’s Caeleigh again!
We are so happy to see all of you engaging and posting on our aphasia group blog! Olivia, Christina, and I are enjoying your research about aphasia facts! This is what this blog is all about- sharing information and experiences. This is also a way to combat boredom!
Christina mentioned a movie on Netflix called My Beautiful, Broken Brain. We thought we would share information about this movie with you as something to reflect upon over the weekend if you get a chance to watch it. When Christina mentioned this movie, I thought, “ah yes, I love this movie!” I watched it a few years ago while getting my Bachelor’s degree at University at Buffalo during midterms week as a way to “take a break” (if you can call it that after watching this movie…) from studying. It reminded me all over again about why I chose to pursue being a speech-language pathologist- I just have such a heart for people with communication obstacles! I believe that access to communication is extremely important, and this documentary gave me an insight on experiences of someone who struggles with communication.
This documentary (a true story) is about a woman named Lotje Sodderland who suffered from a hemorrhagic stroke (i.e., brain bleed) as a result of a congenital vascular malformation (i.e., growth in the blood circulatory system that is present at birth) at the age of 34. She describes her experience of aphasia as if she is living in a David Lynch film. David Lynch is a film producer that creates movies and television series that are artistic and confusing. If any of you have seen Twin Peaks (a television show from the 1990s), this is a television series by David Lynch (also available on Netflix). It is quite a strange and other-worldly type of show, and one of my favorites! This is how Lotje describes her experience having aphasia. Ultimately, Lotje submitted her idea for this documentary to David Lynch and he produced My Beautiful Broken Brain. Throughout the duration of the film, Lotje describes different treatments she endures to improve her communication through speaking, reading, and writing. She also discusses her journey of embracing her world with aphasia. It is quite an incredible film!

Another movie that I have seen that might spark your interest is called Brain on Fire, which is also available on Netflix. This movie is not about a person who has survived a stroke, but about a woman named Susannah Cahalan who suffered from an autoimmune disease that presented itself with similar symptoms of stroke. In this film, doctors were able to resolve her symptoms through medications. Although she may not have had the same diagnosis many of you may experience, this film is still an interesting story! It is based off of a memoir by Susannah Cahalan (so it is a true story too)!
Susannah slowly started experiencing symptoms such as hyper-sensitivity to sound and difficulty maintaining attention. Although she experienced symptoms some of you have not experienced (such as psychosis and hallucinations), she ultimately had difficulty with communication and left-visual field neglect (i.e., difficulty seeing the left side of your environment).
Maybe this is a different story than what you have experienced, but also interesting to bring awareness to other brain complications that someone might experience!
These movies may be something for you to engage in over the weekend! Grab some popcorn and a blanket, and bring your thoughts next Friday!
Caeleigh Heavey, B.A.
Graduate Student Clinician